The Health Benefits of Eating Enough: Why Nourishment Matters in Lifestyle Medicine

For years, many people were taught that “healthy eating” meant eating less. Less food. Fewer calories. Smaller portions. More control. More restriction. And while there are certainly times when nutrition changes are needed for health, the cultural message around food has often become far too simple—and far too harsh. Many people have absorbed the idea that hunger is discipline, skipping meals is success, and feeling underfed is just part of “being healthy.” Now, with the rise of weight-loss medications and renewed cultural focus on rapid weight loss, we are seeing some of those same old messages return in a new form. For some people, medications like GLP-1s can be appropriate and life-changing when used with medical guidance. But the broader cultural conversation can sometimes drift back toward something unhealthy: eat as little as possible, shrink yourself quickly, and treat appetite like the enemy. From a Lifestyle Medicine perspective, that is not the goal. Food is not just something to restrict. Food is information. Food is fuel. Food is nourishment. Food is one of the most powerful ways we support energy, mood, muscle, hormones, blood sugar, digestion, inflammation, and long-term health. And many people are surprised to learn this: when you are eating the right kinds of foods, you can often eat a lot more than you think. Eating Well Does Not Always Mean Eating Less One of the most important shifts in nutrition is moving away from the question, “How little can I eat?” and toward the question, “How well can I nourish my body?” There is a big difference between eating a small amount of highly processed food and eating a full plate of whole, nutrient-dense food. A small amount of ultra-processed food may be high in calories but low in fiber, protein, volume, and nutrients. It may not keep you full for long. It may leave your blood sugar less stable. It may trigger cravings or make you feel like you are constantly trying to “be good.” On the other hand, meals built around vegetables, beans, lentils, whole grains, fruit, nuts, seeds, and quality proteins can often be much more satisfying. These foods tend to bring more fiber, more volume, more micronutrients, and more steady fuel. That means eating well may actually look like eating more food—not less. More color.More plants.More fiber.More protein.More minerals.More satisfaction.More support for the body you are living in. Undereating Can Work Against Your Health When people are trying to improve their health, it is easy to assume that cutting back is always the answer. But chronically undereating can create real problems. Not eating enough can affect: Your body needs enough fuel to function. If you are constantly under-eating, your body may respond by increasing cravings, lowering energy, disrupting sleep, making workouts feel harder, and pushing you toward quick energy foods later in the day. This is one reason restriction can become such a frustrating cycle. You try to eat very little.You feel tired and deprived.Cravings increase.You overeat or feel out of control.Then you blame yourself and start restricting again. But often the problem is not a lack of willpower. The problem is that the body is underfed. Food Is Foundational to Energy If you are tired all the time, food is not the only thing to look at—but it is absolutely one of the foundations. Your body needs steady fuel to make energy. That means enough overall food, but also the right balance of nutrients. Meals that include protein, fiber-rich carbohydrates, healthy fats, and colorful plant foods can help support steadier energy throughout the day. This may look like oatmeal with nuts and berries, a bean and vegetable soup, a grain bowl with roasted vegetables and tofu, eggs with greens and whole-grain toast, or a hearty salad with beans, avocado, and seeds. The goal is not to eat perfectly. The goal is to give your body something to work with. When meals are too small or too low in nutrients, it is common to feel shaky, foggy, irritable, or exhausted. Many people then reach for caffeine or sugar—not because they are failing, but because the body is asking for energy. Eating enough, especially earlier in the day, can make a meaningful difference. Eating Enough Helps Stabilize Cravings Cravings are often treated like a character flaw. But many cravings are physiological. If you skip breakfast, under-eat at lunch, push through the afternoon with coffee, and then feel ravenous at night, that is not a personal failure. That is a body trying to catch up. Eating enough during the day can help reduce the intensity of evening cravings. Protein, fiber, and complex carbohydrates are especially helpful because they support fullness and more stable blood sugar. This does not mean cravings will disappear forever. Food is emotional, social, cultural, and pleasurable too. But when the body is consistently nourished, cravings often become easier to understand and work with. Instead of asking, “Why do I have no self-control?” you can ask, “Did I actually eat enough today?” That question alone can change everything. Nourishment Supports Hormones and Metabolism The body does not experience food restriction in isolation. When you do not eat enough, especially over time, the body may interpret that as stress. This can affect hormones, thyroid function, reproductive health, sleep, mood, and metabolism. For women in perimenopause and menopause, nourishment becomes even more important. This stage of life already brings hormonal changes that can affect muscle, body composition, sleep, mood, insulin sensitivity, and energy. Under-fueling the body during this time can make those challenges harder. This is one reason I encourage women to think beyond weight loss alone. The question is not just, “How can I get smaller?” The better question is, “How can I stay strong, nourished, energized, and metabolically healthy as I age?” That requires enough food.Enough protein.Enough fiber.Enough minerals.Enough strength-building support.Enough care. Eating Enough Helps Protect Muscle Muscle is one of the most important tissues for long-term health. It supports strength, balance, mobility, metabolism, insulin sensitivity, bone health, and independence as
The Quiet Middle: What Happens After You Decide to Start an NP Practice

There is a lot of energy around the beginning of a dream. You imagine the kind of practice you want to build. You think about the patients you want to serve, the care you want to offer, the freedom you want to create, and the way your work could finally feel more aligned with who you are as a provider. That part can feel exciting. And then there is the other side. The quiet middle. The place after you have decided you want to start an NP practice, but before you feel fully established. Before the schedule is full. Before the systems are smooth. Before your website feels perfect. Before you have answers to every question. This is the stage where many nurse practitioners start to wonder, “Am I really cut out for this?” Not because they are incapable. Because the quiet middle is where the dream becomes real work. The Quiet Middle Is Where the Details Show Up Once you move beyond the idea of starting a practice, the details begin to surface. What services will you offer? Will you take insurance, stay cash pay, or create a hybrid model? What will your first appointment include? How long should your visits be? What should you charge? What needs to be on your website? How will patients schedule? What forms do you need? What policies should be in place? How will you handle follow-up questions, refills, labs, cancellations, and communication between visits? None of these questions mean you are doing anything wrong. They are simply part of building a practice. But when you are in the middle of it, the number of decisions can feel overwhelming. You may find yourself spending an hour trying to write one paragraph for your website. Or going back and forth on pricing. Or comparing scheduling platforms. Or wondering whether your offer is clear enough. Or second-guessing a choice you felt confident about yesterday. That is the quiet middle. It is not glamorous, but it is important. Doubt Often Gets Louder in This Stage Many NPs expect doubt before they decide to start. But sometimes doubt actually gets louder after the decision has been made. That can feel confusing. You finally chose to move forward, so why do you suddenly feel less confident? Because now the idea is no longer theoretical. Now you are making real choices. Real money is involved. Real patients may be reading your words. Real people may ask questions. Real systems need to support the kind of care you want to provide. That can bring up a lot. What if no one books? What if I charge too much? What if I charge too little? What if I choose the wrong model? What if my website sounds awkward? What if I forget something important? What if I am not ready? These questions are common. They are also not proof that you should stop. They are often just signs that you are moving from dreaming into building. You Do Not Need to Feel Certain About Everything One of the hardest parts of the quiet middle is wanting certainty before you move forward. You may want to know your perfect niche, perfect pricing, perfect schedule, perfect software, perfect wording, and perfect long-term plan before you take the next step. But private practice does not usually come together that way. You learn by building. You learn by trying something, noticing what works, adjusting what does not, and letting your practice become clearer over time. Your first version does not have to be your forever version. Your first service does not have to define your entire career. Your first website does not have to say everything perfectly. Your first office space does not have to be the dream space. Your first schedule does not have to be the schedule you keep forever. The goal is not to make every decision perfectly. The goal is to make thoughtful decisions that allow you to keep moving. This Stage Requires a Different Kind of Confidence The quiet middle asks for a different kind of confidence than clinical practice. In clinical care, confidence often comes from training, experience, repetition, and knowing what to do when something presents in front of you. In business, confidence is a little different. It is the confidence to make a decision without having every answer. It is the confidence to write the website copy even if it feels imperfect. It is the confidence to choose a price and revisit it later. It is the confidence to create a simple offer instead of trying to explain every possible thing you can do. It is the confidence to ask for help. It is the confidence to keep going through the awkward parts. That kind of confidence is built slowly. Not by waiting until you feel fearless, but by taking the next manageable step. The Quiet Middle Is Where Your Practice Starts to Take Shape Even though this stage can feel messy, it is also where your practice begins to become real. Every small decision gives your business more form. Choosing your services gives patients a clearer way to understand how you can help. Writing your website helps you clarify your voice. Creating policies helps protect your time and energy. Setting prices helps make the practice sustainable. Choosing systems helps create a better experience for both you and your patients. Deciding your schedule helps your business fit your actual life. These details may not feel as exciting as the original dream, but they are what make the dream functional. A practice is not built only from vision. It is built from decisions, systems, boundaries, communication, and consistency. You Are Allowed to Start Small One of the most supportive things you can do in the quiet middle is simplify. You do not have to launch with every service you may eventually want to offer. You do not have to have a full-time office. You do not have to create a massive program. You do not have to
Sleep Hygiene from an NP’s Perspective

Sleep is one of the most underrated foundations of health. As a nurse practitioner, I often see how deeply sleep affects energy, mood, hormones, blood sugar balance, pain, cravings, immune function, and the ability to follow through with healthy habits. When sleep is off, everything can feel harder. You may find yourself reaching for more caffeine, craving more sugar, feeling less motivated to move your body, struggling with emotional regulation, or feeling like you are “failing” at habits that might actually be much more manageable with better rest. Sleep hygiene is not about creating a perfect bedtime routine. It is about building conditions that help your brain and body recognize when it is time to wind down, restore, and repair. Why Sleep Matters So Much Sleep is not passive. Your body is doing essential work while you rest. During sleep, your nervous system has a chance to shift out of constant alert mode. Your brain processes information, supports memory, and clears metabolic waste. Your immune system becomes more active. Hormones involved in hunger, fullness, stress, blood sugar, and tissue repair are regulated. When sleep is consistently too short or poor quality, the effects often show up throughout the entire body. People may notice more inflammation, more anxiety, more irritability, more pain sensitivity, higher cravings, lower resilience, and more difficulty making health-supportive choices. This is one reason sleep is such an important pillar of Lifestyle Medicine. It supports almost every other area of health. Start with Your Wake-Up Time One of the most helpful sleep habits is often not about bedtime at all. It is about wake-up time. Waking up around the same time each day helps anchor your circadian rhythm, which is your body’s internal clock. This rhythm influences when you feel alert, when you feel sleepy, when certain hormones rise and fall, and how your body responds to light, food, movement, and stress. If your sleep schedule is irregular, start by choosing a realistic wake-up time and keeping it fairly consistent, even on weekends. You do not have to be perfect, but consistency helps your body learn a rhythm. Once your wake-up time becomes more predictable, bedtime often becomes easier to adjust. Get Morning Light Morning light is one of the strongest signals for your circadian rhythm. Getting outside soon after waking, even for a few minutes, can help tell your brain, “This is daytime.” Natural light helps regulate melatonin timing, supports daytime alertness, and can make it easier to feel sleepy later in the evening. This does not have to be complicated. Step outside with your coffee or tea. Take a short walk. Sit near bright natural light. Open the curtains. The goal is to give your body a clear morning signal. This can be especially helpful during darker months, when many people notice lower energy, mood changes, or disrupted sleep patterns. Be Thoughtful with Caffeine Caffeine can be a helpful tool, but it can also quietly interfere with sleep. Many people can fall asleep after caffeine and assume it is not affecting them, but caffeine can still reduce sleep quality, increase nighttime awakenings, or decrease the amount of deep sleep they get. A good starting place is to avoid caffeine later in the day, especially in the afternoon and evening. Some people need an even earlier cutoff. This depends on genetics, stress levels, hormones, medications, and overall sensitivity. If sleep has been a struggle, consider experimenting with your caffeine timing before assuming you need a more complicated solution. Create a Wind-Down Routine Your nervous system usually needs transition time. Many people go from work, caregiving, screens, chores, or stress directly into bed and then wonder why their mind is still racing. A wind-down routine gives your body a chance to shift gears. This might include dimming the lights, stretching, taking a warm shower, reading, journaling, listening to calming music, practicing breathwork, or doing a quiet evening ritual that feels realistic for your life. The goal is not to perform a perfect routine. The goal is repetition. When you repeat the same calming cues over time, your brain begins to associate them with sleep. Protect Your Bedroom Environment Your sleep environment matters. A cool, dark, quiet room is ideal for most people. Light exposure at night can interfere with melatonin, especially bright overhead lighting or screens close to the face. Noise, temperature, pets, and clutter can also affect sleep quality. Simple changes can help: blackout curtains, an eye mask, earplugs, white noise, breathable bedding, or lowering the thermostat. Your bedroom does not need to look like a spa. It just needs to support rest. Watch the Evening Scroll Screens are not only an issue because of blue light. They are also stimulating. Scrolling, checking email, watching intense content, reading upsetting news, or getting into emotionally charged conversations can keep the brain alert long after the phone is put away. If you use screens at night, consider creating a softer boundary. This might mean setting a cutoff time, using night mode, avoiding work email, or choosing calming content instead of anything activating. A helpful question is: “Is this helping my body feel safe enough to sleep?” Consider Food, Alcohol, and Late-Night Habits What happens in the evening can influence sleep. Going to bed overly full may worsen reflux or discomfort. Going to bed hungry may also disrupt sleep. Alcohol may make you feel sleepy at first, but it often fragments sleep later in the night and can reduce sleep quality. A balanced evening meal, enough protein and fiber during the day, and a gentle nighttime routine can all support more stable sleep. For some people, a small evening snack can help. For others, finishing food earlier works better. This is where individualized care matters. When Sleep Hygiene Is Not Enough Sleep hygiene is powerful, but it is not the whole story. If someone is doing “all the right things” and still struggling, it may be time to look deeper. Insomnia, anxiety, depression, chronic pain, perimenopause, thyroid changes, restless
How to Learn the Business Side of NP Practice

For many nurse practitioners, the clinical side of practice feels familiar. You know how to listen, assess, diagnose, educate, prescribe, support, and follow up. You know how to hold space for patients and help them move toward better health. But the business side of NP practice can feel like a completely different language. Pricing. Marketing. Policies. Scheduling. Documentation systems. Business structure. Bookkeeping. Billing. Website copy. Patient flow. Legal considerations. Office space. Insurance. Cash pay models. Contracts. Boundaries. It can feel overwhelming at first, especially if you were never taught any of this in school. Many NPs leave training with strong clinical skills but very little preparation for how to actually build and run a practice. That does not mean you cannot learn it. The business side of NP practice is not magic. It is not something only “business-minded” people can understand. It is a collection of skills, decisions, systems, and habits that can be learned one step at a time. You Do Not Have to Know Everything Before You Start One of the biggest mistakes NPs make when thinking about private practice is believing they need to understand every part of business before they take a first step. They think they need the perfect business plan, the perfect website, the perfect pricing structure, the perfect office, the perfect niche, and the perfect long-term vision before they begin. But most successful practices are not built from perfect certainty. They are built through thoughtful action, real-world learning, and steady refinement. You do need to be responsible. You do need to understand your legal, ethical, clinical, and financial obligations. You do need to practice within your scope and set yourself up safely. But you do not need to have every detail figured out on day one. There is a difference between being prepared and waiting until you feel completely fearless. Most NPs never feel completely ready. Confidence often grows after you start taking the next right steps. Start by Understanding the Kind of Practice You Want to Build Before you get lost in business details, it helps to step back and ask a bigger question: What kind of practice are you actually trying to create? Not just what services you could offer, but what kind of professional life you want to build. Do you want a small, quiet practice with a limited number of patients? Do you want a busy insurance-based clinic with a larger team? Do you want to offer telehealth? Do you want to combine medication management with lifestyle medicine, functional medicine, women’s health, mental health, hormone care, primary care, coaching, or another specialty? Do you want to work full time, part time, or slowly build while keeping another job? Do you want employees, or would you rather stay small and simple? Do you want a brick-and-mortar office, a shared space, a virtual model, or a hybrid approach? These questions matter because the business side of NP practice is not one-size-fits-all. A solo cash-pay practice has different needs than an insurance-based primary care clinic. A telehealth practice has different systems than an in-person wellness practice. A part-time practice has different financial expectations than a full-time clinic with staff. Learning business becomes easier when you are not trying to learn everything at once. You are learning what applies to the kind of practice you actually want to build. Learn the Basic Business Pieces One at a Time The business side of NP practice can feel overwhelming because people tend to lump it all together. But it becomes more manageable when you separate it into categories. There is the legal and structural side: business formation, scope of practice, collaborating or supervising requirements if applicable in your state, professional liability coverage, policies, consent forms, HIPAA, documentation, and compliance. There is the financial side: startup costs, pricing, revenue goals, bookkeeping, taxes, payment systems, billing, insurance contracts if you use them, and understanding how much money the practice needs to bring in to be sustainable. There is the operational side: scheduling, patient communication, charting, forms, follow-up systems, prescription workflows, lab processes, referrals, and day-to-day organization. There is the marketing side: your website, messaging, social media, networking, referral relationships, email list, local visibility, and helping the right people understand what you offer. There is also the leadership side: decision-making, boundaries, time management, patient expectations, and learning how to be both a clinician and a business owner. You do not have to master all of these at once. Start with the pieces that matter most for your next phase. If you are still dreaming, you may need clarity and basic education. If you are preparing to launch, you may need structure, startup steps, and professional guidance. If you are already open, you may need help refining systems, marketing, or sustainability. Get Comfortable With Money Many NPs are deeply caring, service-oriented people. That is one of the strengths of the profession. But when you own a practice, you also have to be willing to talk about money. This can feel uncomfortable at first. You may wonder what to charge. You may worry that your rates are too high. You may feel guilty asking patients to pay directly. You may avoid looking closely at the numbers because they feel intimidating. But money is not separate from care. Your practice has to be financially sustainable in order to keep serving people. Learning the business side of NP practice means learning how to understand your costs, your time, your capacity, and your revenue needs. It means recognizing that your clinical expertise has value. It means creating a structure that supports both your patients and your own wellbeing. This does not mean you have to become money-driven. It means you have to become financially clear. A practice that undercharges, overextends, or avoids financial planning will eventually feel stressful and unsustainable. A practice with thoughtful pricing, clear policies, and realistic expectations is more likely to last. Learn Marketing as Education and Connection Marketing is another area that can feel uncomfortable for many NPs.
The Importance of Building and Maintaining Muscle
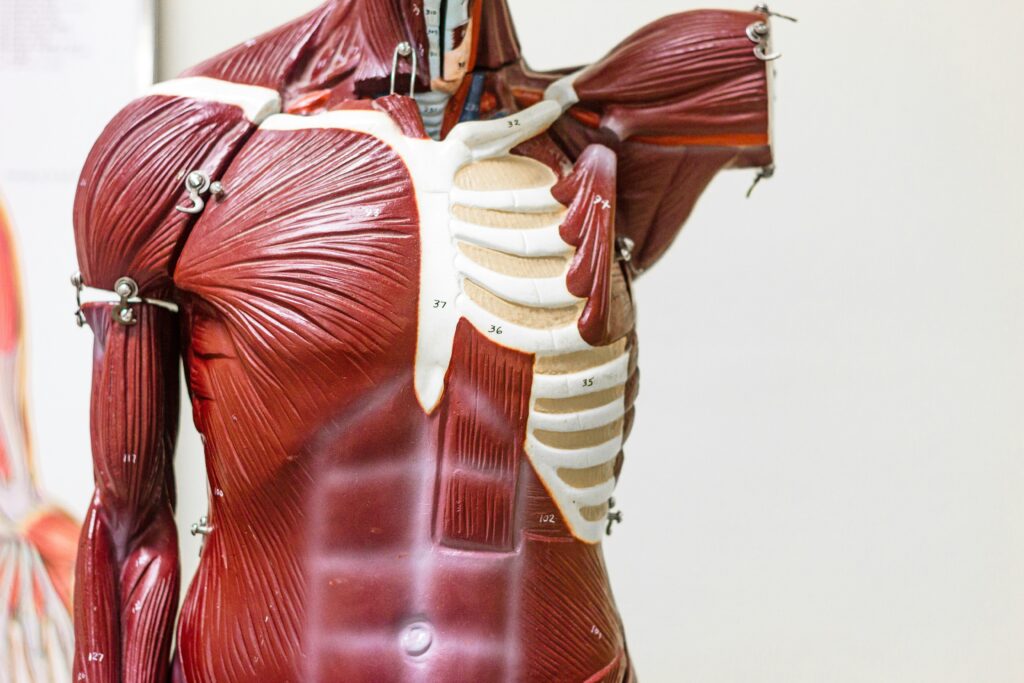
When many people think about muscle, they think about appearance, fitness goals, or time spent at the gym. But muscle is much more than that. Building and maintaining muscle is one of the most important things women can do to support long-term health, energy, mobility, metabolism, bone health, and independence. From a Lifestyle Medicine perspective, strength is not about chasing a certain body type. It is about supporting the body so it can keep doing the things that matter: walking, lifting, carrying, climbing stairs, playing with kids or grandkids, traveling, gardening, dancing, and moving through daily life with more ease and confidence. Muscle is part of the foundation that helps us age well, feel steady in our bodies, and maintain our quality of life over time. Muscle Supports Everyday Strength Strength training does not only matter for athletes or people who love the gym. It matters for everyday life. We use muscle every time we carry groceries, lift a laundry basket, get up from a chair, climb stairs, open a heavy door, walk uphill, or get up from the floor. When we have more strength, these everyday tasks often feel easier and safer. Maintaining muscle also supports balance, posture, and coordination. This becomes especially important as we get older, when falls and injuries can have a bigger impact on independence and quality of life. Building muscle is not about becoming extreme. It is about creating enough strength to feel capable in your own body. Muscle and Healthy Aging As we age, we naturally begin to lose muscle mass unless we actively work to maintain it. This age-related muscle loss can affect strength, mobility, metabolism, and overall function. For women, this can become especially noticeable during midlife and beyond. Hormonal changes, changes in activity level, stress, sleep disruption, and busy caregiving or work demands can all make it easier to lose muscle and harder to rebuild it. The good news is that muscle is responsive. With consistent movement, strength training, adequate protein, recovery, and supportive lifestyle habits, the body can build and maintain strength at many stages of life. It is never too late to begin. Even small, steady efforts can make a meaningful difference over time. Muscle Supports Bone Health Strength training is also important for bone health. This matters deeply for women, especially as bone density can decline with age and hormonal changes. Muscles and bones work together. When muscles pull against bone during resistance exercise, it gives the body a signal to maintain and strengthen bone tissue. Weight-bearing movement and resistance training can support stronger bones and may help reduce the risk of fractures over time. This does not mean every person needs to lift heavy weights right away. Bodyweight exercises, resistance bands, light weights, step-ups, squats, and functional movement can all help create that important signal. The key is consistency and gradual progression. Muscle Helps Support Metabolism and Blood Sugar Balance Muscle also plays an important role in metabolic health. Muscle tissue helps the body use and store glucose, which means maintaining muscle can support healthier blood sugar balance and steadier energy. This is one reason strength training can be such a powerful tool in Lifestyle Medicine. It is not only about burning calories during exercise. It is about building tissue that supports the body’s ability to manage energy, insulin sensitivity, and long-term metabolic health. Muscle also helps support a healthy metabolism as we age. Since muscle is more metabolically active than fat tissue, preserving muscle can help support overall energy use and body composition in a more sustainable way. Again, the goal is not punishment or perfection. It is support. Strength Training Does Not Have to Be Complicated One of the most encouraging things about building muscle is that it does not require an intense gym routine to begin. Strength can be built through simple, approachable movements like squats, wall push-ups, lunges, bridges, step-ups, resistance bands, hand weights, Pilates, strength-focused yoga, gardening, carrying groceries, or short strength sessions at home. For many people, starting with two short strength sessions per week is a realistic and supportive goal. Over time, you can gradually add more resistance, more repetitions, or more challenging movements. The best strength routine is one you can actually keep doing. Protein, Recovery, and Lifestyle Matter Too Movement is important, but muscle also needs support from nutrition and recovery. Protein provides the building blocks needed for muscle repair and maintenance. Many women, especially those eating lighter meals or skipping meals during busy days, may not be getting enough protein spread throughout the day. This does not mean protein needs to become obsessive or complicated. It simply means including nourishing protein sources regularly, such as beans, lentils, tofu, tempeh, eggs, fish, poultry, Greek yogurt, nuts, seeds, or other options that fit your needs and preferences. Sleep and recovery also matter. Muscle is built and repaired during rest, not just during exercise. Chronic stress, poor sleep, under-eating, and overtraining can all make it harder for the body to build and maintain strength. Whole-person health always works together. Strength Is a Form of Self-Care Building muscle is not about trying to look younger, smaller, or more acceptable. It is about caring for your future self. It is about being able to carry what you need to carry. To move with more confidence. To support your bones and joints. To feel more stable and capable. To maintain independence for as long as possible. To have the strength to keep participating in the life you love. For women, strength can be deeply empowering. It can shift the focus away from shrinking the body and toward supporting the body. That shift matters. Start Small and Build From There If strength training feels intimidating, start small. Begin with a few basic movements, a short walk with hills, a resistance band routine, or simple exercises you can do at home. You do not need to overhaul your life in one week. You do not need the perfect plan. You do not need
The Quiet Confidence of Starting Small

So many nurse practitioners wait to begin because they think their practice needs to look fully formed before it can be real. They imagine they need the perfect website, the complete business plan, the polished offer, the professional photos, the booking system, the newsletter, the social media strategy, and a clear answer to every possible question before they take the first step. But most practices are not built all at once. They are built through small, thoughtful decisions repeated over time. You Do Not Need the Perfect Office to Begin Many NPs imagine private practice starting with a beautiful office, a fully decorated treatment room, a front desk, signage, and everything perfectly in place. But your first office does not have to be your forever office. Starting small might look like renting one room a few days a week. It might look like sharing space with another provider. It might look like beginning with a simple, calm, functional room that allows you to provide good care while you learn what you actually need. You can always grow into a larger space later. What matters in the beginning is that the space supports safe, thoughtful care and helps you take the next step. Telehealth Can Be a Simple Starting Point For some nurse practitioners, telehealth can be a practical way to begin without the overhead of a physical office. It may allow you to start with lower costs, a more flexible schedule, and a simpler setup while you clarify your services and build relationships with patients. Of course, telehealth still needs to be done carefully. You need to understand your state rules, licensure requirements, documentation, consent, privacy, and what kinds of care are appropriate virtually. But when it fits your scope and your model, telehealth can be a meaningful way to start small without waiting for every physical detail to be perfect. Your First Offer Can Be Simple You do not need to launch ten services at once. In fact, trying to offer everything can make it harder for people to understand what you do. A small beginning might mean choosing one clear service: a new patient consult, a follow-up package, a lifestyle medicine visit, a hormone support consultation, a wellness-focused appointment, or another offer that fits your training and values. You can refine from there. Your first offer does not have to represent everything your practice will ever become. It just needs to be clear enough for someone to say, “Yes, that is what I need.” Your Systems Can Grow With You It is easy to get stuck thinking you need the perfect EHR, booking system, newsletter platform, intake forms, payment system, and patient workflow before you start. Yes, systems matter. But they can also evolve. In the beginning, you may need something simple, organized, and compliant — not perfect. As you see real patients, you will learn where the friction points are. You will notice what questions come up again and again. You will discover what needs to be automated, clarified, or improved. That feedback is valuable. You cannot always design the perfect system from the outside. Sometimes you have to start, observe, and adjust. Confidence Comes From Taking the Next Real Step Starting small does not mean you are playing small. It means you are giving yourself room to learn, adjust, and grow without the pressure of having everything figured out on day one. A strong practice is not built from one huge leap. It is built from the small decisions you keep making: the room you rent, the telehealth system you test, the offer you clarify, the patient you serve well, the boundary you honor, the message you refine. That is the quiet confidence of starting small. If you’re an APRN dreaming about private practice but feeling overwhelmed by where to start, I can help you take the next thoughtful step through my Business Mentorship for APRNs.
Hydration, Without the Hype

A grounded Lifestyle Medicine look at why hydration is essential, how to support it well, and where hydration products actually fit Hydration is often talked about in one of two extremes. On one end, it gets treated like something so basic it hardly deserves much thought. On the other, it gets turned into a full wellness industry category, packed with powders, sticks, salt blends, and “advanced hydration” promises that make plain water sound outdated. Neither extreme is especially helpful. Hydration is not trivial. It is foundational. It affects temperature regulation, circulation, digestion, physical performance, kidney function, energy, mental clarity, and overall resilience. When hydration is off, people often feel it quickly. Sometimes it shows up as thirst or dry mouth. Other times it looks more like fatigue, headaches, sluggishness, constipation, irritability, or just feeling less functional than usual. From a Lifestyle Medicine perspective, hydration deserves real respect. It is one of the daily basics of health. At the same time, it does not need to be overcomplicated or driven by product marketing. A grounded approach makes room for both truths: hydration is deeply important, and many people can improve it without turning it into a supplement routine. Why hydration is such a big deal Water is not just one healthy habit among many. It is part of how the body functions moment to moment. Hydration supports blood volume, helps move nutrients through the body, assists with waste removal, supports digestion, helps regulate body temperature, and plays a role in how well muscles and the brain perform. When fluid intake falls short, the body has to compensate, and that can affect energy, heat tolerance, mental clarity, and overall physical function. This is why hydration should not be brushed off as a minor wellness tip. It is not just about athletic performance or surviving a hot day. It matters during ordinary life too. It matters when you are working, parenting, exercising, traveling, recovering from illness, or simply trying to feel your best from one day to the next. Even mild underhydration can matter. It does not have to become severe before it starts affecting how you feel. Many people live in a pattern of being a little underhydrated much of the time and simply assume that low energy, headaches, poor exercise tolerance, or sluggish digestion are normal. Hydration is simple in theory, but not always easy in real life In theory, hydration is straightforward: drink enough fluids. In real life, it is easy to fall behind. People get busy. They rely heavily on coffee and forget water. They spend hours indoors without noticing thirst. They work out and do not replace what they lose. They eat fewer water-rich foods than they realize. They travel, drink alcohol, get sick, or spend more time in heat than usual and never really adjust. This is where Lifestyle Medicine offers a helpful lens. It brings us back to patterns instead of quick fixes. Hydration is not just about remembering a water bottle. It is also shaped by your routines, meals, workday, movement, environment, and how attentive you are to your body’s needs. What good hydration actually looks like For most people, good hydration looks less like hitting a perfect number and more like building a strong pattern. It means drinking regularly throughout the day instead of waiting until you feel depleted. It means increasing fluids when you are sweating more, spending time in heat, traveling, or recovering from illness. It means paying attention to thirst, urine color, energy, and physical cues rather than treating hydration like an afterthought. It also means remembering that hydration does not come only from beverages. Food matters too. Fruits, vegetables, soups, smoothies, yogurt, and other water-rich foods can contribute meaningfully to hydration. This is one of the many reasons a minimally processed, plant-forward way of eating supports health on multiple levels at once. That is a very Lifestyle Medicine point: the best support for hydration often overlaps with the same daily habits that support the rest of your health. When hydration starts to slip Many people do not immediately realize when hydration is falling short because the signs can be subtle at first. Sometimes it is obvious, like strong thirst or dark urine. But often it is less dramatic. You may just feel more tired than usual, a little foggy, more headachy, more easily overheated, a bit off during exercise, or less steady in your energy and mood. That does not mean every symptom points to hydration. But it does mean hydration is one of the first basics worth checking when the body is not feeling well-supported. The problem with hydration hype Because hydration is genuinely important, it is easy for marketing to build on that truth. That is where things get distorted. A real physiological need gets turned into the message that everyone needs a branded solution all the time. Water begins to sound inadequate. Electrolyte mixes are framed like daily essentials. Buzzwords like “cellular hydration” get used to make ordinary physiology sound more mysterious than it is. The issue is not that hydration products are worthless. Some absolutely have a place. The issue is when an important health topic gets turned into confusion, fear, or unnecessary dependence on products that may not actually be needed for everyday life. A better question is not, “Is this product healthy?” It is, “What is this product for, and does my situation actually call for it?” A deeper look at hydration products Electrolyte powders and packets Electrolyte products can be useful, but they need context. Electrolytes like sodium and potassium help regulate fluid balance, nerve function, and muscle function. Sodium becomes especially important when you are sweating heavily or losing fluids through illness. In those situations, replacing fluid alone may not always be enough. But that does not mean everyone needs electrolyte powders every day. Some hydration mixes are fairly modest. Others are loaded with sodium. For someone doing prolonged activity in the heat, working outdoors for hours, or losing fluid through
The Biggest Mistake New NPs Make When Thinking About Private Practice

Thinking You Need to Have It All Figured Out One of the biggest mistakes new nurse practitioners make when thinking about private practice is believing they need to have everything figured out before they start. That belief sounds responsible on the surface, but it often keeps people stuck. Many NPs spend months or even years waiting until they feel more confident, more certain, or more prepared. They tell themselves they will move forward once they know exactly what services to offer, what model to choose, what to charge, how to market themselves, and how every part of the business will work. But that is rarely how real progress happens. Why This Mindset Holds So Many NPs Back Nurse practitioners are trained to take their work seriously. You are taught to be thoughtful, careful, and prepared. Those qualities are important in clinical practice, but in business they can sometimes turn into hesitation, perfectionism, and overthinking. Instead of taking the next step, many NPs stay in research mode. They keep gathering information, comparing options, and trying to create the perfect plan before they have enough experience to know what will actually fit them best. The problem is that private practice is not something you fully figure out in advance. It becomes clearer as you move through it. Clarity Comes From Action This is the part many people miss. You do not usually gain confidence first and then take action. More often, confidence grows because you took action. The same is true for clarity. You learn more about your niche by thinking through who you most want to serve. You learn more about your business model by exploring your options. You learn more about your systems and workflow by beginning to map out how you want your practice to function. So much of what feels unclear at the beginning only becomes clearer once you start engaging with the process. That does not mean jumping in recklessly. It means understanding that movement creates information. Waiting forever does not. What You Actually Need at the Beginning You do not need a perfect business plan on day one. You do not need every answer. You do not need to feel fearless. What you do need is a strong foundation and a clear next step. That might mean learning your state requirements, getting clearer on the kind of care you want to offer, thinking through your values, or asking bigger questions about what kind of practice you want to build. It may also mean recognizing where you need support instead of assuming you have to do every part alone. Private practice is built one decision at a time. It is not built by magically becoming fully ready. The Value of Mentorship This is one reason mentorship matters so much for new NPs. When you are trying to sort through business structure, pricing, offers, marketing, legal considerations, and the emotional weight of doing something new, it is easy to get overwhelmed. Mentorship helps you focus on what matters most right now instead of spiraling over everything at once. It can also help you stop mistaking uncertainty for incapability. Having questions does not mean you are not cut out for private practice. It usually means you are in the early stages of building something important. A Better Way to Move Forward Instead of asking, “Do I have everything figured out?” a better question is, “What is my next right step?” That question creates momentum. It shifts your focus from perfection to progress. And progress is what actually builds a practice. If private practice is something you keep thinking about, do not let uncertainty convince you that you are not ready. You may not need a flawless plan. You may simply need support, a clearer starting point, and the willingness to begin. The biggest mistake is not being new. The biggest mistake is assuming you have to know everything before you start. If you are looking for support as you navigate the path toward private practice, explore my Business Mentorship for APRNs.
Lifestyle Medicine, Protein, and Plant-Based Eating: What Really Matters?

Protein is everywhere right now. It’s in smoothies, snack bars, chips, coffee drinks, and social media posts telling us to pile more of it onto every plate. And while protein is important, the conversation has gotten a little louder than it is helpful. In many cases, protein is being marketed as the answer to everything, when the real picture is much more nuanced. From a Lifestyle Medicine perspective, protein matters, but so does context. It’s not just about how much you eat. It’s also about where it comes from, what comes with it, and how it fits into your overall pattern of eating. Why Protein Matters Protein plays an important role in the body. It helps support muscle maintenance, tissue repair, hormone production, immune function, and steady energy. It can also help meals feel more satisfying, which is one reason people often feel better when they start being more intentional about including it. This is especially important during certain seasons of life, like aging, recovery, times of higher physical demand, or when working on maintaining strength and function. Protein is not something to ignore. But that does not mean more is always better. When Protein Becomes a Trend Instead of a Tool One of the biggest problems with nutrition trends is that they often take something important and turn it into something exaggerated. That is exactly what has happened with protein. Yes, protein matters. But many people are already getting enough. The bigger issue is often the overall quality of the diet, not a dramatic lack of protein. In fact, some people become so focused on hitting high protein targets that they lose sight of other things the body also needs, like fiber, variety, healthy fats, and minimally processed foods. Protein should support a healthy way of eating. It should not become the whole strategy. The Lifestyle Medicine View Lifestyle Medicine looks at the bigger picture. Instead of asking only, “How can I eat more protein?” it asks, “What kind of eating pattern supports long-term health?” That shift matters. A protein-rich diet made up mostly of processed convenience foods is very different from a diet that includes protein through whole, nourishing foods that also support heart health, blood sugar balance, digestion, and inflammation. This is one reason plant-based protein deserves more attention. Why Plant-Based Protein Is Worth Talking About Plant-based proteins do more than provide protein alone. Foods like beans, lentils, tofu, tempeh, edamame, nuts, seeds, and whole grains often come packaged with fiber, vitamins, minerals, and protective plant compounds that support health on multiple levels. That is one of the strengths of plant-based eating. These foods are not just helping you meet a protein goal. They are also supporting gut health, heart health, metabolic health, and fullness in a way that many ultra-processed “high protein” products simply do not. In other words, the source matters. Plant-Based Protein Options to Build Meals Around There are so many simple ways to include more plant-based protein in everyday life without overcomplicating it. Some great options include: These foods can be used in soups, grain bowls, salads, stir-fries, tacos, curries, breakfasts, and snacks. They are versatile, affordable, and easy to build into meals over time. What About “Complete” Protein? This is one of the most common concerns people have when they start leaning more plant-based. Animal proteins are often described as “complete” because they contain all the essential amino acids in amounts the body can use easily. Some plant foods are lower in certain amino acids, but that does not mean plant-based eating is inadequate. When you eat a variety of plant foods throughout the day, your body can still get what it needs. You do not need to perfectly combine foods at every meal or obsess over matching amino acids on your plate. A varied, balanced approach usually does the job very well. Not Everything With Protein Is Healthy This is another place where the current trend can get confusing. Just because a food is high in protein does not automatically make it nourishing. A highly processed snack with added protein is still a highly processed snack. Marketing can make it sound like a health food, but a “protein” label does not erase the bigger picture. That does not mean those products can never have a place. It just means they should not become the foundation of your nutrition. Whole foods still matter most. A More Balanced Way to Think About Protein A healthier approach is to stop treating protein like a competition. You do not need to chase extreme numbers. You do not need to force protein powder into everything. And you do not need to be afraid that every plant-based meal is somehow falling short. Instead, aim for meals that are balanced, satisfying, and built from real food. Include protein regularly. Consider plant-based options more often. Pay attention to how your body feels. And remember that nutrition is about patterns, not perfection. What This Can Look Like in Real Life This might mean adding lentils to soup, black beans to tacos, tofu to a stir-fry, hemp seeds to oatmeal, or edamame to lunch. It might mean swapping in a bean-based meal a few times a week or simply broadening your definition of what counts as a solid protein source. Small shifts add up. You do not have to do everything at once to move in a healthier direction. The Bottom Line Protein is important. But it is also a little overhyped right now. Most people do not need to panic about getting more and more of it. What they often need instead is a more balanced, whole-food approach that includes enough protein while also making room for fiber, variety, and foods that truly support long-term health. That is where plant-based protein shines. It offers nourishment that goes beyond grams alone, and it fits beautifully into a Lifestyle Medicine approach that values the whole person, the whole plate, and the long game of health. If you are looking for a
LLC vs PLLC for Nurse Practitioners: What’s the Difference?

If you are a nurse practitioner thinking about starting your own practice, you may have come across two terms that sound almost the same: LLC and PLLC. It is an easy point of confusion, especially when you are already trying to navigate business setup, legal requirements, and the many moving pieces that come with private practice. The good news is that the difference is actually pretty simple once you break it down. What’s the Difference? An LLC, or limited liability company, is a common business structure used by many small businesses. A PLLC, or professional limited liability company, is a similar structure that is specifically used in some states for licensed professionals. Since nurse practitioners are licensed providers, some states may require a PLLC instead of a standard LLC when an NP is opening a clinical practice. That is the main difference: an LLC is a general business structure, while a PLLC is designed for certain licensed professions. Why This Matters for Nurse Practitioners For nurse practitioners, the biggest thing to understand is that this is often a state-specific issue. In one state, an NP may be allowed to form an LLC. In another, a PLLC may be required. That is why there is not one universal answer for everyone. This is also why it is important not to rely too heavily on what another provider did in a different state. What worked for them may not be the right fit for your situation. What an LLC or PLLC Does Not Do It is also important to understand what these structures do and do not do. Forming an LLC or PLLC can help create a legal separation between you and your business in certain situations, but it does not mean you are personally protected from your own malpractice. That is why choosing a business structure is only one part of building your practice well. Malpractice insurance, legal guidance, and financial support still matter. Questions to Ask Before You Choose If you are trying to decide between an LLC and a PLLC, here are a few important questions to ask: These questions can help you get clearer on what applies to your practice before you file anything. Final Thoughts The bottom line is this: if you are a nurse practitioner starting a private practice, the choice between an LLC and a PLLC usually comes down to the rules in your state and the type of services you plan to offer. Starting your own practice comes with a lot of decisions, and this is one of those foundational ones that is worth getting right from the beginning. You do not need to have everything figured out all at once, but taking the time to understand your options can save you stress later. And you do not have to figure it all out alone. Business Mentorship for APRNs